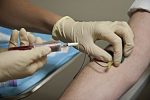
Therapeutic phlebotomy is a type of treatment for people who have too much iron in their body. You may not think that too much iron is a bad thing, but excessive amounts can be harmful. Various conditions can cause an excess of iron, and they need to be kept under control.
For some people, blood can be overloaded with different components. It’s important to have the right amounts of iron, specifically, in your blood. Too much can cause significant health risks and can even lead to other potential diseases.
Therapeutic phlebotomy isn’t much different on the surface as getting blood drawn for any other reason. But, there is a specific purpose behind it. It also has to be specially ordered by a doctor. It’s not the same as a general blood draw where many different things are tested.
You may have heard of an iron deficiency. But, having too much iron in the blood can be as dangerous. If you’ve ever been told your iron levels are high, you may want to talk to discuss the possibility of a therapeutic phlebotomy treatment. If you’re looking into a career in phlebotomy, it’s important to know how therapeutic phlebotomy works and how to do it the right way.
[su_list icon=”icon: check-circle”]
Do I Need a Therapeutic Phlebotomy Procedure?
This guide will cover the ins and outs of therapeutic phlebotomy. You’ll find that many of the actions are the same as getting your blood drawn for anything else. But, there are specific rules and protocols to follow.
Phlebotomists need to know the differences between a regular blood draw and therapeutic phlebotomy. We will cover what you should know about performing it, as well as what side effects your patients might experience because of the procedure.
What Are the Reasons for Therapeutic Phlebotomy?
Therapeutic phlebotomy can be a life-saving treatment for patients with too much iron in their blood. This is a condition called hemochromatosis. Your body needs a certain amount of iron. It’s used to make hemoglobin, which oxygenates your cells. But, like anything else, there can be too much of a ‘good thing’ when it comes to iron in the blood.
When you have too much iron in your blood, it can cause damage to your heart or liver. It can lead to diseases like diabetes or arthritis. These are severe conditions that should be looked at and treated as soon as possible.
So, how can you tell if you might have too much iron in your blood? If you get regular blood tests or yearly checkups, your doctor should be able to notice elevated iron levels and recommend treatment.
But, other symptoms include things like:
- Joint pain
- Fatigue
- Abdominal pain
- Irregular heartbeat
- Changes to skin color
As you can see, some of these symptoms can be quite serious and scary. If you’re experiencing any of them, it’s important to get your blood tested right away. There are other conditions that therapeutic phlebotomy is used for as well.
Hough hemochromatosis is the most common, others include:
- Polycythemia vera – Increased bone marrow that can lead to higher blood viscosity. Thicker blood usually means you have too much blood in circulation. But, getting regular draws can help. The danger of having blood with high viscosity is that it can create problems with clotting.
- Sickle cell disease – This occurs when red blood cells are misshapen or tend to break down. Therapeutic phlebotomy can help by lowering blood viscosity and reducing the concentration of the affected red blood cells in one area.
- Porphyria – This is caused by too much porphyrin in the blood. Too much of it can affect the nervous system, cause gastrointestinal pain, or affect the skin. Therapeutic phlebotomy can help to remove excess amounts of porphyrin. It’s a condition that can’t be cured, but things like phlebotomy can help to manage it and keep symptoms from becoming severe.

It’s important to understand that for many of these conditions, there is no cure. Whether a doctor offers several types of treatment or just one, therapeutic phlebotomy isn’t designed to cure a blood disorder completely. Some people have to go through the procedure many times in their life.
It’s used as more of a management tool. It can help to ease painful symptoms or allow someone to live a normal life. For most people, it isn’t a quick fix or one-time solution.
Therapeutic Phlebotomy Guidelines
If you’re someone who regularly donates blood, you might think you don’t need something like therapeutic phlebotomy. But, if you have one of the conditions above, the designated time between blood donation draws is too long. The least amount of time between draws is 56 days by a community blood bank. For someone with too much iron in their blood or another condition, symptoms can become severe during that time.
A prescription is needed from a physician to take part in therapeutic blood drawing. This is because it needs to happen more frequently than what a typical blood donation draw would be. The physician will do everything from recommending how often the blood should be drawn to how much of it should be taken each time.
Therapeutic phlebotomy protocol needs to be followed by whoever is drawing the blood. They need to get consent from the patient, and they need to follow the direct orders from the physician. This type of phlebotomy can be done for a patient until their doctor has seen that the levels of iron in their body have balanced out. Once that ‘goal’ is achieved, most patients can maintain healthy iron levels by donating blood regularly at local blood banks.
Guidelines can differ based on where a patient goes for this procedure. Most blood banks have a similar protocol and rules that phlebotomists need to follow.
These typically include:
- The phlebotomist must follow every order from the prescription. This includes how much blood should be drawn and the frequency of bleeding.
- No more than 500 ccs of blood should ever be taken at one time. Occasionally, a prescription may request 1000+ ccs. In these cases, schedule the patient’s second draw no sooner than 72 hours after their first draw. Anything closer than that must be approved by a licensed Pathologist.
- Always use a blood pressure cuff to track the patient.
- Explain to the patient how the procedure will be performed. Most hospitals and blood banks need the patient sign a form once it is explained to them.
Can Someone with Too Much Iron Donate Blood?
If you have hemochromatosis, you might wonder if your blood is viable for use. The good news is that there is no reason your blood can’t be used to help save lives. Hemochromatosis is not considered a blood disorder. Instead, it’s a metabolic disorder.
Unfortunately, many hospitals and clinics across the country discard the blood drawn for therapeutic purposes. It can still help to save your life and keep you healthy by getting it drawn. But, you won’t be able to donate it to someone else. If you’re a phlebotomist who works in a hospital like this, making sure you follow the standard safety procedures for discarding blood is essential.
If you’re a phlebotomist who wants to work for a community blood center, you may be able to help someone with too much iron donate their blood to others. Many blood banks across the country do this. Each one varies on what they allow. So, whether you’re a donor or the person drawing the blood, choose a location that fits with your personal needs and ethics.
[/su_list]
How to Perform Therapeutic Phlebotomy
Many of the steps to performing therapeutic phlebotomy are just like a standard blood draw. First, the amount of blood taken is usually a lot more than what is taken for a lab sample. Second, the needle for therapeutic phlebotomy is typically a little larger. This keeps the red blood cells from becoming damaged as the blood is drawn.
Other than those two significant differences, the steps are as follows:
- A site is chosen for the blood draw. Usually, it’s a vein located on the arm, around the bend where your elbow is. Sometimes, you may need to find a different site if you don’t have a viable vein there.
- The area is cleaned using an antiseptic.
- The larger needle is inserted into the vein, and the blood draw begins.
- A phlebotomy technician will remove the designated amount of blood as prescribed by a doctor. For therapeutic phlebotomy, this is usually anywhere from 450-500 milliliters. That equals about one pint of blood.
- Once the right amount of blood has been drawn, the needle is removed. The area is once again cleaned, and typically, a small band-aid is put over the site of the needle to prevent further bleeding.

Blood needs to be collected in a transfer pack at a rate that’s comfortable for a patient. To get a pint of blood, this usually takes anywhere from 10-15 minutes. For some patients, it can take longer. It’s important to check on the patient while the blood is being transferred to make sure it’s not flowing at a rate that is too quick for them.
Can Children Be Treated with Therapeutic Phlebotomy?
Children can have the same medical conditions as adults, including the ones that therapeutic phlebotomy can help to treat. Many children’s hospitals and regular hospitals treat children who have too much iron in their blood. Or, they may have other conditions that need it.
As with any physician, a child’s doctor will have to determine the amount of blood that should be drawn. Therapeutic phlebotomy for a child may take longer because their blood shouldn’t be drawn as quickly. It can take an hour or two for some children.
When it comes to therapeutic phlebotomy for children, it’s not unlikely for a physician or specialist to be with the parents and child while the blood draw is taking place. Most children’s hospitals offer this ‘service.’ It tends to ease the discomforts of the parents and child. The physician can answer questions and put everyone’s mind at ease by making sure the entire procedure is going smoothly.
The procedure can regularly be performed as prescribed by the child’s doctor. It may be a procedure that needs to happen for years for the child to live normally.
[su_list icon=”icon: check-circle”]
What Are the Possible Side Effects?
For the most part, therapeutic phlebotomy is entirely safe. Most of the risks involve a user-error. As a phlebotomist, it’s important to understand those risks. You are taking responsibility for someone’s well-being with every blood draw.
Aside from the risks associated with phlebotomy, some patients may experience some of the following side effects:
- Nausea
- Dizziness
- Vomiting
- Bruising
- Pain at the injection site
Many of the side effects are just like what someone might experience after donating blood. Many times, some of these side effects can be lessened or avoided by treating your patients the same way as you would for a blood donation. This includes making sure they’ve eaten something beforehand and are adequately hydrated.
Some patients will feel better if they have something to snack on during or after the procedure, too. It’s vital that they stay hydrated, as well. These simple measures can help most patients avoid things like dizziness or even fainting spells due to a loss of blood.
For some people, a saline solution is pumped into the body to replace the fluid that’s coming out. This is an especially common practice for children who undergo therapeutic phlebotomy.
What Are the Other Benefits of Therapeutic Phlebotomy?
Aside from helping with high levels of iron and helping to balance out other conditions of the blood, there are many benefits. Keep in mind that this type of phlebotomy is different from donating blood. Donating blood can be hugely beneficial to you, and others! But, therapeutic phlebotomy is something that requires a prescription.
If you’re a candidate for that kind of prescription, you can experience some of the following benefits:
- Many patients who undergo therapeutic phlebotomy say they feel better, in general, after having the procedure. This is usually due to the removal of toxins from the body. An iron buildup can also leave you feeling lousy in a lot of ways. Just one session of therapeutic phlebotomy can make a lot of those negative symptoms go away or not feel as severe.
- It helps to clear your circulatory system. Because of this, it can help some people who suffer from hypertension. It may also help to lower blood pressure and dangerous cholesterol levels.
- Therapeutic phlebotomy gives your spleen a break! It’s the job of your spleen to filter blood and remove old red blood cells. It can work overtime if you’re producing too many red blood cells or if your blood has a high viscosity. This procedure can allow your spleen to rest for a while and let it perform its natural functions without having to work harder than usual.
- Many different kinds of toxins can be removed from your body through regular therapeutic phlebotomy. Not only can this help you feel better, as stated above, but it can help your body function better. Think of it as a ‘tune-up.’ Your organs can function at a higher level when a buildup of toxins is removed.
- Therapeutic phlebotomy can stimulate your bone marrow. As a result, your bone marrow will be triggered to produce new, healthy red blood cells.
Of course, these benefits are bonuses to why therapeutic phlebotomy is good for you. The most important thing is making sure a blood condition doesn’t take over or ruin your life. Getting blood regularly drawn via a doctor’s request can prevent that from happening and give you the benefits listed here, too.
Is Extra Training Required to Perform Therapeutic Phlebotomy?
Phlebotomy has always been needed in the healthcare field. But, in recent years it has become a favorite career. This is because more tests have been made available through blood draws. Phlebotomy is considered an entry-level job in healthcare, so a lot of people are interested in it. Even to become a certified phlebotomist, training typically takes less than a year.
In this training period, the time is typically split in two. Some of the time will be spent in a classroom setting. A phlebotomist needs to learn everything from human anatomy and the different systems of the body to safety procedures. The rest of the time will be spent practicing blood draws (venipuncture). A phlebotomy student needs to complete a certain amount of successful blood draws to complete a training program. This number varies from school to school but is usually well over 100.
If you want to perform therapeutic phlebotomy, extra training is required. This is due to the slight differences in typical blood draws and therapeutic blood draws. A therapeutic phlebotomist will need to take more training courses. These courses have to be specific to therapeutic phlebotomy. A separate certification exam is also required for this kind of procedure. To keep up your certification, you’ll consistently need to get more education credits over the years. It can be a lot of work, especially for an entry-level position.
While this extra training can take more time, it also comes with benefits. There are fewer therapeutic phlebotomists than traditional phlebotomy techs. So, your position will have a higher demand. You may be more likely to get hired since you can perform both types of phlebotomy.
Taking the time to get extra training also usually comes with a pay raise. Most phlebotomists who can also do therapeutic phlebotomy make more money than ‘regular’ phlebotomy technicians.
Where Can a Therapeutic Phlebotomist Work?
A phlebotomist who can perform therapeutic phlebotomy can work just about anywhere a traditional phlebotomy tech works. A majority of certified phlebotomists work in hospitals. This is even more common for therapeutic phlebotomists since the draws they perform have to be prescribed by a doctor.
A therapeutic phlebotomist can also work for clinics or private practices. They can even work for blood banks and donation centers. If you have certification in therapeutic phlebotomy, your skills can be used in many different venues. This includes locations that many others might not even think about, like nursing homes or homeless shelters.
Some phlebotomists take their skills and continue to use them on a volunteer basis from time to time. Again, there is a growing demand for phlebotomists all over the country. If you have extra skills and certifications, you’ll be in greater demand from those who have certain blood conditions and need help.
Should I Become a Therapeutic Phlebotomist?
Becoming a phlebotomist is a great way to enter the medical field. You can either use it as a stepping stone to more advanced medical positions or turn it into a life-long career. Traditional phlebotomy can help patients when it comes to diagnosing potential health issues. Or, they can make sure everything is normal in a patient’s blood.
A therapeutic phlebotomist, though, can benefit specific patients. Patients who are struggling with blood disorders need this kind of therapy to keep their symptoms at bay. It can take a little extra time and training to become certified as a therapeutic phlebotomist. But, the increase in salary and demand are often worth it for people who are already interested in phlebotomy.
If you’ve never heard of therapeutic phlebotomy or wanted to know more about it, we hope this guide has been helpful. It’s certainly not a new practice, but, it’s not yet as popular as traditional phlebotomy. It’s a great time to get into this particular field and help a lot of people along the way. Most phlebotomy programs across the country will offer several courses on therapeutic phlebotomy, so it’s not hard to get started right away.
[/su_list]